Menu
- (206) 207-1525
- (206)207-1625
- info@seattlejawsurgery.com
Coming Soon!
Coming Soon!
Traditionally, if your orthodontist suspects that you may need jaw surgery you will be referred for a jaw surgery consultation prior to the initiation of your orthodontic treatment. At that time we will discuss the surgical options that are available and the typical timeline. After your consultation with our office your orthodontist will begin your orthodontic treatment. Keep in mind that you will typically be in braces for 6 months to 2 years prior to your jaw surgery. When you are ready for surgery your orthodontist will notify you and our office. We will see you in clinic 2-3 months prior to your planned surgical date to be sure that we are ready for your surgery. You will be seen in our clinic one additional time 2-3 weeks prior to surgery for your pre-operative appointment. After your surgery is completed you can expect to spend one night in the hospital. Typically patients are discharged home the day after surgery. We will then see you for follow up appointments at 1 week, 3 weeks, 6 weeks and 6 months. About six weeks after your surgery your orthodontist will see you and begin the final stages of your orthodontic treatment to fine tune your teeth.
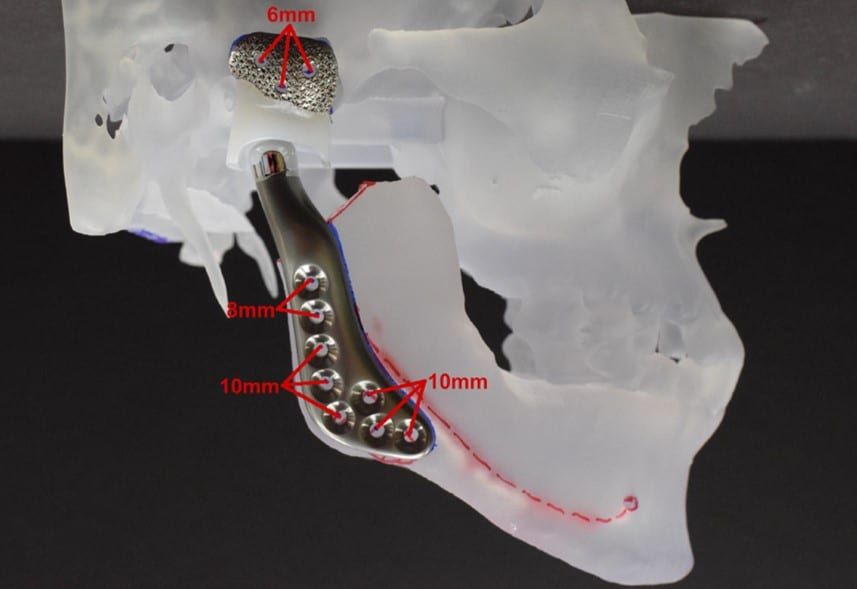
Joint replacement is a commonly performed surgical procedure. Each year in America, hundreds of thousands of knees, hips, and shoulders are replaced. For the temporomandibular joint (TMJ), it is more unusual. Many patients can benefit from the procedure. For TMJ, replacement is useful for patients with severe arthritis, severely limited mouth opening (ankylosis), joint tumors, trauma, infection, or failed previous devices.
Many times, issues with the joint can influence the overall function of the entire lower jaw. The goal for TMJ replacement is to restore function of the jaw joints. Replacing the TMJ can help reduce pain, improve mouth opening, make your upper airway bigger, correct a poor occlusion, and improve facial balance. Overall, our focus is to allow patients to improve their quality of life.
Dr. Bobek is known in the Pacific Northwest for his surgical expertise with TMJ joint replacement. He uses TMJ Concepts which fabricates custom titanium joints based on the patient’s actual anatomy. This allows for a customized and precise surgical planning with positive patient outcomes.
Recovery after joint replacement can take several weeks to months. After surgery, patients will spend 1-2 nights in the hospital and are followed in clinic with post-operative appointments at 1, 3 and 6 weeks. Patients start TMJ physical therapy about 2 weeks after surgery. At this time, they can generally return to work and begin many normal jaw functions. Given the core functions that the TMJ supports, we generally estimate that it takes 6 months before patients stabilize into their new normal state following joint replacement.
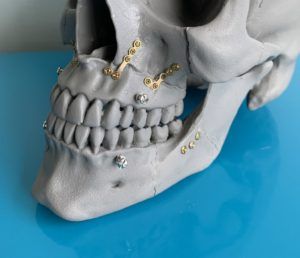
Orthognathic Surgery is the medical term for Jaw Surgery. It is a surgery to reposition the jaws to correct alignment. This realignment allows teeth to fit when misalignment cannot be solved by orthodontics alone.
Jaw surgery is completed at the hospital under general anesthesia. It is used to treat several conditions including a severe underbite or overbite, open bite, jaw or facial asymmetry, sleep apnea and others.
Typically, patients find themselves in our office after seeing an orthodontist. The orthodontist will make the recommendation based on your jaw alignment and teeth alignment if surgery may be needed in addition to orthodontic treatment to correct your bite. They would refer you to discuss orthognathic surgery with a maxillofacial surgeon.
Your initial consult in our clinic will consist of one of our surgeons taking a history, doing an examination, reviewing your clinical photos and any available imaging. They will then discuss what is involved with jaw surgery and anticipated surgical intervention. You will also be shown a cartoon demonstration video of how jaw surgery is used to reposition the jaws. After this consult you return to your orthodontist to begin orthodontic treatment.
The traditional timeline for jaw surgery patients is to be in braces for a period of time, on average this is about 6-18 months to straighten and align the teeth prior to surgery. Then the orthodontist will tell the patient when they are close to being ready for surgery. It is then that you follow up in clinic for a recall visit. One of our maxillofacial surgeons will do another exam and we will take updated photos. The surgeon will then have a better idea of what surgical treatment they recommend. At this recall if you are ready for surgery you will meet with one of our care coordinators to schedule a surgery date.
You return to clinic to obtain presurgical records. These records include an updated CT scan and an optical scan of your teeth. These are used by the surgeons to complete your virtual surgical planning (VSP). This is a way to customize the surgery to each individual patient. At your preoperative visit we will discuss the process of surgery at the hospital, review your specific plan for surgery, and review instructions for recovery after surgery.
Surgery takes place at the hospital; you spend one night in the hospital after surgery and are discharged the following day. We see you in clinic for your post operative visits at 1, 3, and 6 weeks after surgery and then 6 months after surgery.

Coming Soon!
Coming Soon!
Coming Soon!
